A study called a lung CT has become widely known in the context of the COVID-19 pandemic. However, it can detect much more than the changes related to the notorious virus. In fact, chest CT is used to identify a whole range of conditions - from inflammation to neoplasms. But in addition to the benefits, the method also has certain risks and limitations. How can you make the best of its advantages and reduce the potential dangers?
What is a CT scan of the lungs?
The term «tomography» implies the creation of layer-by-layer images (scans). In the case of CT scans, they are obtained using X-rays due to the fact that body tissues absorb them in different ways. First, several cross-sectional images of the study area are taken at various angles, which are then combined into a high-resolution three-dimensional image. Processing is carried out with the help of a computer program. To see the lungs, the scanner target area is the chest.
Computed tompgraohy often serves as a supplement to conventional X-rays.
Indications
CT of the lungs is used to diagnose a number of abnormalities. Compared to X-rays, it is characterized by a much higher resolution and three-dimensionality, which makes it possible to identify even very fine structures in the lung tissue.
This scanning method is especially often used to detect tumors and metastases, as well as to monitor the disease after therapy. In addition, the technique is effective for the diagnosis of numerous inflammatory conditions. Apart from classic pneumonia, chronic obstructive pulmonary disease (COPD) can be diagnosed.
The study (or rather, its variation, called CT angiography) is also applicable in visualizing pulmonary arteries. In this way, both occlusions (e.g., in the case of pulmonary embolism) and vascular changes (e.g., atherosclerosis-related ones, or aneurysms) can be clearly identified.
Last but not least, chest CT is also used when planning major surgeries in the sternal region, as it can clearly show the relevant structures.
The best way to obtain additional information in all forms of acute and chronic lung disease is high-resolution computed tomography (HRCT). In this case thin (not thicker than 1.2 mm) slices are created, which allow a particularly good view of the lung tissue, with a reduction in radiation exposure of up to 50%.
| Condition | Typical CT-Pattern |
| Pulmonary Embolism (PE) | Дефект наполнения контраста; четкая визуализация тромба |
| Pneumonia | Areas of tissue thickening (ground-glass opacity). |
| Lung Cancer |
Light-colored areas of tissue transmitting less X-rays; increased vascular pattern, single ground-glass opacity spots. |
| COPD | «Air traps» (areas of increased airiness, dilation, deformation and dense bronchial walls. |
| Fibrosis | «Cellular» lung (lineups of uniform air-containing cysts). |
What is the proper procedure to get ready for a lung CT scan and why is it important?
Patient preparation is an important prerequisite for optimal results. The key aspects requiring maximum attention are:
- assessment of the state of the kidneys and thyroid function;
- understanding how to behave immediately before and during the procedure;
- eating and water intake before and after the scan.
Why does your renal function matter?
Iodine-based radiopaque contrast agents are used to better visualize tissue (e.g., to evaluate the blood vessels or detect atypical blood flow patterns in malignant tumors). They are excreted from the body through the kidneys. Under certain conditions (first of all, if kidney failure already exists), the risk of complications, such as the development of nephropathy caused by the contrast agent, increases. Therefore, preparation for a lung CT scan with contrast includes a creatinine level blood test.
Why should you check your thyroid before a contrast-enhanced lung CT?
To identify such risks, a TSH (thyroid stimulating hormone) blood test is performed in preparation for a contrast CT scan. In case of abnormalities, additional precautions may be required, such as blockade of hormone production with certain medications.
No jewelry or metal objects!
Patient behavior directly affects the quality and accuracy of CT images. Image errors and motion artifacts make them difficult to interpret. Jewelry, implants and cosmetics containing metal also pose a problem for radiologic examinations. Therefore, wristwatches, hearing aids, eyeglasses, jewelry, etc. should be removed before the examination.
Are there restrictions on food and water intake?
When contrast administration is planned, you should refrain from eating solid food and consume only non-carbonated liquids (water, black tea) for 3-4 hours before the procedure to avoid nausea. Patients suffering from diabetes mellitus should agree in advance with their physician to take appropriate medications.
After the procedure, it is allowed to eat and drink as usual. Moreover, after a contrast-enhanced scan, it is recommended to drink plenty of water to accelerate the elimination of the substance from the body.
What happens before a lung CT scan?
Before the examination you will talk to your doctor. The main issues to be discussed shall include:
- Risks associated with this type of examination.
- Your current medications. Interaction of some drugs (such as metformin prescribed for diabetes) with the contrast agent may result in kidney damage.
- Chronic diseases, such as metabolic disorders.
- Known intolerances and allergies.
- Pregnancy: due to radiation exposure, computed tomography in pregnant women should only be performed in exceptional emergency cases. Therefore, women of childbearing age should inform the medical staff of an existing (or possible) pregnancy.
In most facilities, patients getting ready for a chest CT are encouraged to avoid mealst within 6 hours before the examination to ensure better image quality.
What happens during the scanning?
The patient is placed on a special table, which is gradually moved into the scanner. During the procedure, the X-ray tube and detector system rotate around the patient to produce single slice images. Compared to an MRI machine, the tube of this tool is so short that a person can look out of it during the study, and claustrophobia is not usually felt. However, sedation may be administered prior to the procedure.
No third persons are allowed in the exam room; you can reach the staff any time via intercom. In ultrafast multidetector spiral computed tomography, the lung tissue is examined without gaps in 1-3 mm thick slices during a breath hold of 12-15 seconds. Holding your breath is necessary to ensure good image quality and to display the lungs in an expanded view.
Certain medical situations require the use of a contrast agent, which is administered approximately 1 hour before the procedure.
Is contrast always necessary?
Iodine-containing contrast agent improves the representation of blood-supplied structures. Inflammations and tumors, in particular, acquire a deep white color after the injection, and can be distinguished from their surroundings. In addition, the method is applicable in pulmonary embolism diagnosis because it ensures a clear color distinction between the blood and the thrombus.
Duration of a chest CT
CT is a simple and quick diagnostic imaging procedure. For this reason, it is often preferred over MRI. The speed also makes it more suitable in emergency situations.
Depending on the purpose, the examination takes between 5 and 30 minutes, but the usual duration is about 10 to 20 minutes. However, the administration of a contrast agent can increase the time by a few more minutes.
Radiation exposure during Chest CT
The study involves a much higher level of radiation than conventional radiography. Radiation exposure depends on the number and thickness of slices, as well as the structure of the tissues being examined. On average, a chest CT scan exposes the patient to about 6-10 millisieverts (mSv). For comparison, the average annual radiation exposure for the average German resident is 2.1 mSv.
This means that the overall likelihood of health damage is low, still the method should only be used if other, lower-risk modalities such as ultrasound or conventional radiography fail to provide sufficient information.
The benefits and risks should be weighed on a case-by-case basis and compared with the advantages and disadvantages of other imaging procedures.
Here are examples:
- Modulation of tube current – by up to 80%
- Automated dose adjustment to individual anatomy - by about 30%
- Image noise reducing solid-state sensors - by about 25%.
Low-dose CT (LDCT) of the lungs as a preventive measure
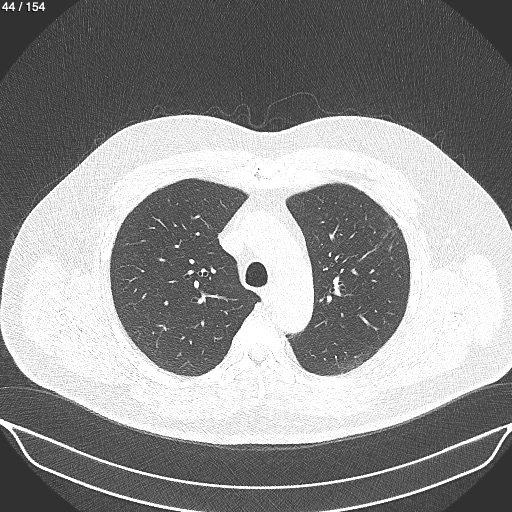
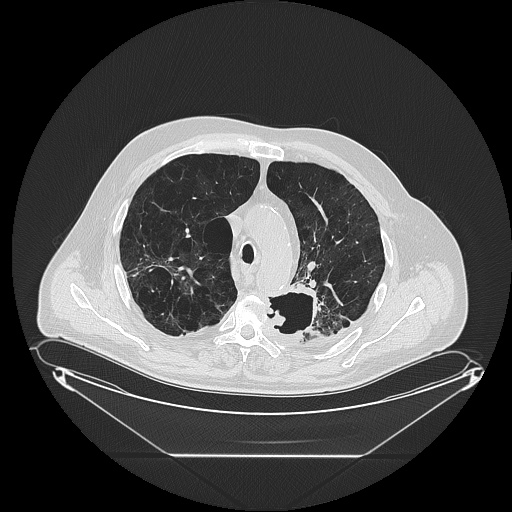
In smokers with a significantly increased risk of developing bronchial carcinoma, low-dose computed tomography can currently be performed instead of chest X-ray for the timely detection of malignant tumors. Due to certain technical improvements, this procedure involves a minimal radiation dose - only 10-30% of a conventional chest CT scan. No contrast agent administration is required.
In the ELCAP (Early Lung Cancer Action Project) study conducted in the USA, it was proved that this method is much more effective than others. Routine lung radiography detects only 14% of small tumors that are detected by CT. If its low-dose modality is used in regular preventive screening, many more cases of cancer can be treated early. Also encouraging is the fact that almost 50% of smokers who participated in the studies subsequently changed their behavior: 23% quit smoking, 27% significantly reduced their smoking!
Another case of lung NDCT application is screening diagnostics in those who have professional contact with asbestos dust.
Result evaluation
The images obtained during the examination are usually reviewed by the doctor immediately afterwards. He or she can usually report the first results immediately. However, since up to 100 images can be produced in total, the doctor shall issue a written report upon detailed evaluation.
A computer-aided detection (CAD) system assists radiologists in the assessment of findings. It examines the patient's CT scan data for possible tumors. The system measures possible lung nodules three-dimensionally (volumetrically), so it is particularly suitable for assessing the progression of small lung nodules. The report is usually sent to the treating physician within a few days.
References:
- S. Diederich. Hochauflösende Computertomographie der Lunge. Milchglas und seine Differenzialdiagnosen. Radiologe. 2010; 50(12): 1141–1152. Published online 2010 Oct 28.
- Camila Piza Purysko, MD, Rahul Renapurkar, MD and Michael A. Bolen, MD. When does chest CT require contrast enhancement? Cleveland Clinic Journal of Medicine June 2016, 83 (6) 423-426; DOI: https://doi.org/10.3949/ccjm.83a.15037
- Mazzone PJ, Silvestri GA, Souter LH, Caverly TJ, Kanne JP, Katki HA, Wiener RS, Detterbeck FC. Screening for lung cancer: CHEST guideline and expert panel report. Chest 2021; S0012-3692(21)01307-6. DOI: 10.1016/j.chest.2021.06.063

Comments — 0